My Concussion Worsened Instead of Getting Better
Written by |

Friday, Sept. 18 is National Concussion Awareness Day. To raise more awareness of how dangerous concussions can be, I’m sharing the most difficult experience of my life. This is the first in a two-part series.
***
OK, I will admit it. I was wrong.
I’ve probably never been more wrong in my life than when I wrote in April, “This was when I knew I finally had made it past the worst of my concussion symptoms.”
I was so naive.
I’ve always felt the need to soften the blows of my reality when sharing my story. I never want to make someone else’s heart hurt because of the horrors I’ve lived through. However, if I protect readers from the reality of how serious my concussion became, I won’t be doing concussion survivors any favors.
The truth of the matter is that my concussion almost killed me. On the last day of June, my speech and heart function suddenly became compromised.
Prior to that, as I was counting down the days to the June 26 anniversary of my first column for Lambert-Eaton News, things started to go awry. I slept and napped constantly. No matter how much I wanted to, I couldn’t stay on top of the most basic chores around my house. The inability to even run my vacuum cleaner caused my décor style to become “à la fur.”
Over the past several years, I’ve learned to live with the fluctuating energy levels caused by my Lambert-Eaton myasthenic syndrome (LEMS), and I attributed my energy challenges to LEMS.
My Lambert-Eaton News Forums co-moderator, Ashley Gregory, was getting concerned. She knew something was very off. She was just one of many friends who knew I wasn’t acting like myself.
I messaged my neurologist almost weekly. Every complaint was met with statements such as “post-concussion syndrome can last for six months” or was not responded to at all. I was begging for help and told to rest.
Then, my writing became affected.
My God-given gift is the ability to write and guide readers along the path of my words to a conclusion or a feeling. I think of my editors here at Bionews, Lambert-Eaton News‘ parent company, as makeup artists. They take something that has great bones, and with a few strokes of expertise, turn out a more polished product. My writing has never looked better than after passing by editors before publication.
Suddenly, with each successive column I wrote in June, my editor needed to rework most of it. Instead of receiving a couple sentences of feedback, I found paragraphs of feedback waiting. This is when I knew I absolutely was not healed from my concussion and requested a couple weeks off in July to rest and hopefully get my brain working again.
Around this time, some extreme emotions came at me from all angles. Anger over a well-respected friend getting fired, excitement over meeting the sweetest rescue dog ever, sadness over helping a homeless gentleman in my hometown of Bangor, Maine. Oh, and all of the stressors we are all dealing with this year, too.
Not once had my neurologist, primary care provider, or the emergency room doctor told me I should try to avoid extreme emotions with a concussion. However, with the way my body and brain were reacting, I knew those emotions had set off a storm of dysfunction in my body.
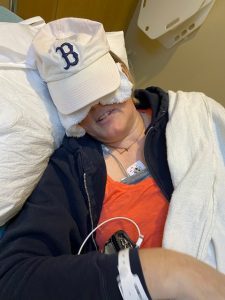
Words spinning in my brain and extreme heart palpitations prompted me to call 911 for the first time in my life. The problem was that I couldn’t respond to their questions. I cried, “I can’t talk, I have post-concussion syndrome.” These words were not spoken evenly, but in a sing-song with pauses. I couldn’t talk normally.
When I was taken out of my house on a stretcher and the EMT asked me questions, I still couldn’t respond. He said, “Fine, refuse treatment.”
Questioning continued in the ER with me crying that I couldn’t answer them. The lights and beeping heart monitors caused searing pain in my brain. My normally extremely low blood pressure soared to 196/118.
My first post-concussion CT scan was performed that day, and fortunately showed no bleeds, shifts, or tumors in my brain. So, despite my ongoing pleas for help, my neurologist suggested a mental health exam. My son and I waited over six hours in the dark for the consultation. I waited because I simply wanted to know what was wrong.
The psychologist was pleasantly surprised when we talked. I told him to read my column and was sent home to rest with the simple diagnosis of “post-concussion syndrome.” My emergency room summary stated I had been seen for migraine.
In the next column, I’ll share details about the scariest month of my life when the dysfunction my body showed at the ER led to a near-death experience.
***
Note: Lambert-Eaton News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Lambert-Eaton News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to Lambert-Eaton myasthenia.





Leave a comment
Fill in the required fields to post. Your email address will not be published.